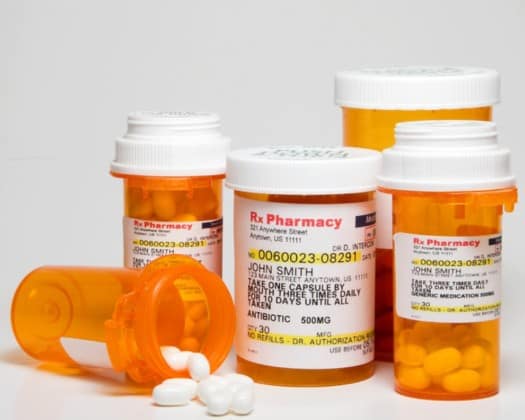
Pharmacy Benefit Managers (PBMs) are known as the “drug middlemen” in America’s system of fulfilling prescriptions for drugs.
PBMs claim that they save consumers money by offering drugs at a rebate price.
And they are quick to tell you that they save “x” percentage on the price, but we consumers never feel the savings, as prices always are going up.
Governor Ron DeSantis, three years ago, put a bullseye on the back of PBMs when he announced in his State of the State speech that drug prices needed to come down and transparency needed to go up.
SB 1550 by Sen. Jason Brodeur (R-Lake Mary) and Rep. Linda Chaney (R-Tampa), who carried the bill in the House, was eventually signed into law.
The bill had good intentions, but some of the abuses that were occurring then are still happening now.
In the meantime, neighborhood, independent pharmacies, the proverbial Mom and Pop business, are struggling to survive the predatory and abusive practices of PBMs.
The Florida Office of Insurance Regulation (OIR), on January 15, 2026, released its “Pharmacy Benefit Managers Examinations Summary Report,” and it was a damning indictment of Florida PBMs.
Under SB 1550, every PBM that does business in Florida must register with the state, and OIR must “examine the business and affairs of each PBM at least biennially” with a “systematic review to determine each PBMs compliance with…all other laws or rules applicable to PBMs.”
To be precise, this is not a performance audit; it is simply an initial examination to ensure that PBMs are operating according to our state law.
Yet, according to OIR, “the Pharmaceutical Care Management Association (PCMA) and TransparencyRx (TransRx), filed petitions challenging the validity of certain actions of the OIR related to PBMs.”
All right. Everyone has the right to ensure that the rules of the road are fair.
But according to OIR, “While the OIR has operated in good faith and made adjustments to the regulations of both PCMA and TransRx have yet to withdraw these challenges,” and to twist the knife further, “…several PBMs have attempted to delay their exams through litigation and responsiveness.”
So, three years after the bill became law, and nine months after the OIR examinations were initiated, many PBMs are still fighting the compliance rules.
As litigation has steadily progressed, OIR indicates that “Neither TransRx nor PCMA have provided language to OIR that it believes is satisfactory. OIR is currently litigating these challenges and waiting for language from either party that might resolve their concerns.” [Editor’s note: some compromise language was finally delivered to OIR after this Report was released, and we do not yet know if OIR is accepting the language.]
The OIR Report goes on to indicate that “34 of the 38 examinations remain active. The completion of certain examinations is delayed because the PBMs have not provided the required contracts or documents for review or due to unpaid invoices relating to examinations owed to examiners.”
To add insult to injury, the Report goes on to state that “8 PBMs exam status is ‘impeded,’ meaning that the PBM examinations are “unable to be finalized due to PBM failure to provide necessary documents or access to their systems” and these PBMs may incur administrative penalties.
Five (5) PBMs are in “settlement litigation,” which means that these PBMs are still involved in pending litigation, and they also may incur administrative penalties.
The Report also shows that collectively 20 PBMs owe over $485,000 to the state for the examination fees, in some cases for over a year.
Yet these same PBMs own some of the top insurance companies in the world, and together they had over $1.1 trillion in revenue in 2025, and the PBMs made over $432 billion in profits!
But they refuse to pay the examiners for their work.
These PBMs treat Florida just like they treat neighborhood, independent pharmacies.
They delay, impede, refuse to provide documents, litigate, and owe money they refuse to pay.
This is why, on average, two independent pharmacies are closing every week, so far this calendar year.
And hundreds of pharmacies, both PBM-owned and independent, have closed across the state.
When asked two weeks ago before a Senate committee how much of the money the PBMs saved Florida last year, the PCMA representative said she did not know.
This is unbelievable.
Florida policymakers cannot afford to trust PBMs at their word.
Tennessee did not; they recently settled with both CVS/Caremark for a $750,000 penalty and for a $250,000 penalty with Express Scripts, two of the three largest PBMs that together monopolize 80% of the prescription drug marketplace in America.
Recently, the Federal Trade Commission settled with Express Scripts; it is still litigating against Caremark and OptumRx, but the FTC announced that the settlement agreement is projected to save consumers $7 billion over the next 10 years, over the price of some drugs, including insulin.
These actions, along with the need to rein in PBM abuses in Florida, are the reasons that SB 1760 should be strengthened to give OIR prior approval of all PBM contracts, just like OIR has authority over all insurance contracts.
OIR should also be given the ability to make it easy for consumers and pharmacists to file an electronic complaint on their website homepage, and they should then aggregate that data and provide analysis annually to the Senate President, House Speaker, and Governor to assist policymakers in making informed and data-driven decisions going forward.
If PBMs are allowed to do business as usual, all consumers in Florida, but especially Medicaid patients, will continue to suffer from unnecessarily higher prescription drug costs in an opaque system that only plies more cash into the pockets of the greedy PBMs.
Barney Bishop III represents SAPR, Small Business Pharmacies Aligned for Reform, a group of independent pharmacists. He is a former Chief Executive Officer of Associated Industries of Florida (AIF), known as “The Voice of Florida Business.” He is also President and Chief Executive Officer of Barney Bishop Consulting LLC, based in Tallahassee, and can be reached at Barney@BarneyBishop.com